Familial Hypercholesterolemia (FH)
Familial hypercholesterolemia (FH) is a genetic disorder that affects the body's ability to remove low-density lipoprotein (LDL) cholesterol from the bloodstream, leading to elevated cholesterol levels. Approximately 1 in 250 individuals are affected by it, but only about 10% are aware they have it. This condition significantly increases the risk of developing coronary heart disease at a younger age.
A healthy LDL level is less than 100 mg/dL (milligrams per deciliter), however, those with familial hypercholesterolemia can have an LDL of 160mg/dL to 400 mg/dL or higher.
For individuals with FH, diet and regular exercise may not be sufficient to lower cholesterol levels to a healthy range. Medications like statins are often necessary to effectively manage cholesterol levels.
Early detection and treatment of this condition are crucial, as they can reduce your risk of heart disease by approximately 80%.
What causes familial hypercholesterolemia?
Familial hypercholesterolemia commonly arises from mutations in the gene responsible for the LDL cholesterol receptor, which plays a vital role in the removal of LDL cholesterol from your body. Mutations in other genes, including PCSK9 and Apolipoprotein B, can also cause inherited high cholesterol. If you inherit a specific type of mutation in any of these 3 genes, familial hypercholesterolemia can develop.
Familial hypercholesterolemia (FH) is categorized into two types based on how it's inherited
Heterozygous Familial Hypercholesterolemia (HeFH)
HeHF is the most common form of FH and inherited in an autosomal dominant pattern. This means that a person only needs to inherit one copy of the mutated gene, either from one affected parent or as a spontaneous mutation, to develop the condition.
Individuals with HeFH have one normal copy and one mutated copy of the gene responsible for LDL receptor function. As a result, their LDL receptors are less effective in removing LDL cholesterol from the bloodstream, leading to high cholesterol levels.
Medication options for HeFH
- Statins
- Bile acid sequestrants
- PCSK9 inhibitors
- Cholesterol absorption inhibitors (Ezetimibe)
Homozygous Familial Hypercholesterolemia (HoFH)
HoFH is a rare and more severe form of FH. It is inherited in an autosomal recessive pattern, which means that a person must inherit two copies of the mutated gene, one from each parent, to develop the condition. Both copies of the gene responsible for LDL receptor function are mutated (non-functional). As a result, their ability to remove LDL cholesterol from the bloodstream is severely impaired, leading to extremely high cholesterol levels.
Those with homozygous familial hypercholesterolemia may require bypass surgeries at a young age, and without treatment, their life expectancy is significantly reduced, with few surviving beyond their 20s.
Medication options for HeFH
- Statins
- PCSK9 inhibitors
- Mipomersen (injection): It works by reducing the production of apolipoprotein B (apo-B), a protein involved in the formation of LDL cholesterol particles.
- Lomitapide: It works by reducing the production of LDL cholesterol in your liver.
What are the signs and symptoms of FH?
FH is often asymptomatic in its early stages, and individuals may not exhibit obvious signs or symptoms. However, as cholesterol levels remain persistently elevated, particularly LDL cholesterol, various signs, and symptoms may develop over time.
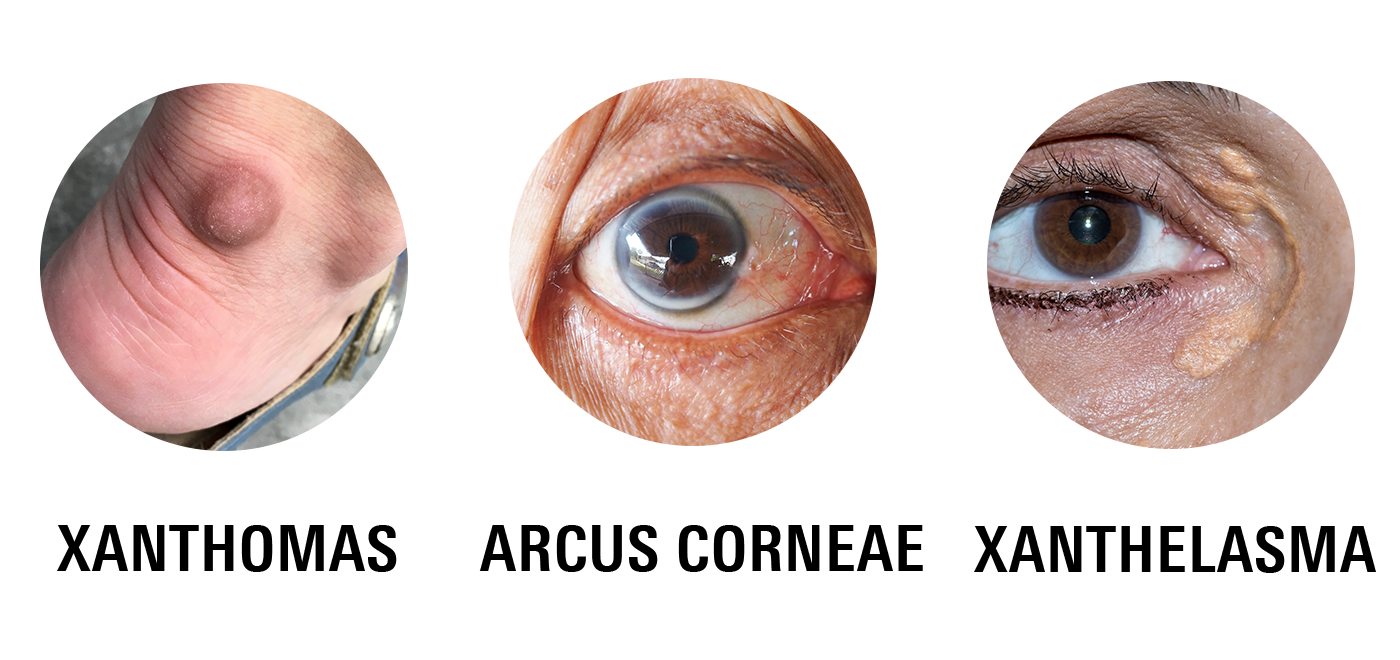
These can include the following:
- Xanthomas: These are deposits of cholesterol that accumulate under your skin. They typically appear as raised, yellowish, and/or whitish bumps or nodules. Xanthomas can occur on various parts of your body, including your tendons, elbows, knees, buttocks, and/ or eyelids.
- Xanthelasma: Refers to the development of cholesterol deposits specifically around your eyelids. These deposits appear as yellowish patches or plaques and can be a distinctive sign of familial hypercholesterolemia.
- Arcus corneae: This involves the presence of a grayish-white ring around the edge of your cornea, the clear front surface of your eye. It can be a sign of elevated cholesterol levels and is more commonly seen in older individuals with familial hypercholesterolemia.
- Premature cardiovascular disease: FH significantly increases your risk of developing cardiovascular disease at an earlier age. Therefore, those with familial hypercholesterolemia may experience symptoms associated with cardiovascular complications, including chest pain, also referred to as angina, shortness of breath, heart palpitations, or even heart attacks.
The severity of familial hypercholesterolemia and its associated symptoms can vary among individuals. Some may have milder forms of familial hypercholesterolemia and exhibit fewer noticeable signs or symptoms, while others may experience more pronounced symptoms.
If there is a concern about familial hypercholesterolemia or elevated cholesterol levels, it’s recommended to consult your doctor for proper evaluation, diagnosis, and management. Genetic testing and lipid profile assessments are often utilized to confirm the diagnosis and assess the risk of cardiovascular disease.
What are the risk factors for FH?
The primary risk factor for familial hypercholesterolemia is having a family history of this condition. Having a parent or close relative with familial hypercholesterolemia significantly increases your risk of developing the condition.
- Genetic Mutations:: FH is caused by specific mutations in genes responsible for regulating LDL cholesterol levels, such as the LDL receptor gene, the apolipoprotein B gene, or the PCSK9 gene. Inheriting one or more of these mutations increases the risk of developing FH.
- Family History: FH is an inherited genetic disorder, so having a family history of the condition significantly increases the risk. If a close family member, such as a parent or sibling, has been diagnosed with FH, the chances of developing the condition are higher.
- Ethnicity: Familial hypercholesterolemia can occur in individuals of all ethnicities and population groups. However, certain populations, including French Canadians, Lebanese, and South African Afrikaners, have a higher prevalence of specific familial hypercholesterolemia genetic mutations.
- Premature Cardiovascular Disease: FH is associated with a significantly higher risk of premature cardiovascular disease, including heart attacks and strokes. If you or a close family member experienced a cardiovascular event at a young age, it may be an indication of FH.
Unfortunately, as of now, complete prevention of familial hypercholesterolemia remains elusive as the genetic mutations responsible for the condition are inherited from affected parents. Nevertheless, early detection and proactive management can significantly reduce your risk of cardiovascular complications associated with familial hypercholesterolemia.
It’s crucial to emphasize the significance of lifestyle modifications, including the adoption of a heart-healthy diet, regular physical activity, weight management, and avoidance of tobacco smoke, as these measures play a pivotal role in managing cholesterol levels and lowering your likelihood of cardiovascular issues.
And although complete prevention is not possible, early diagnosis, effective management, and a comprehensive approach can greatly mitigate the impact of familial hypercholesterolemia, leading to improved long-term outcomes for both individuals affected by this condition and their families.