Medications for COPD
Chronic obstructive pulmonary disease (COPD) is a long-term respiratory disease that causes obstructed airflow from your lungs. The effects of COPD on your lungs cannot be reversed and long-term progression or deterioration results in a steady loss of lung function.
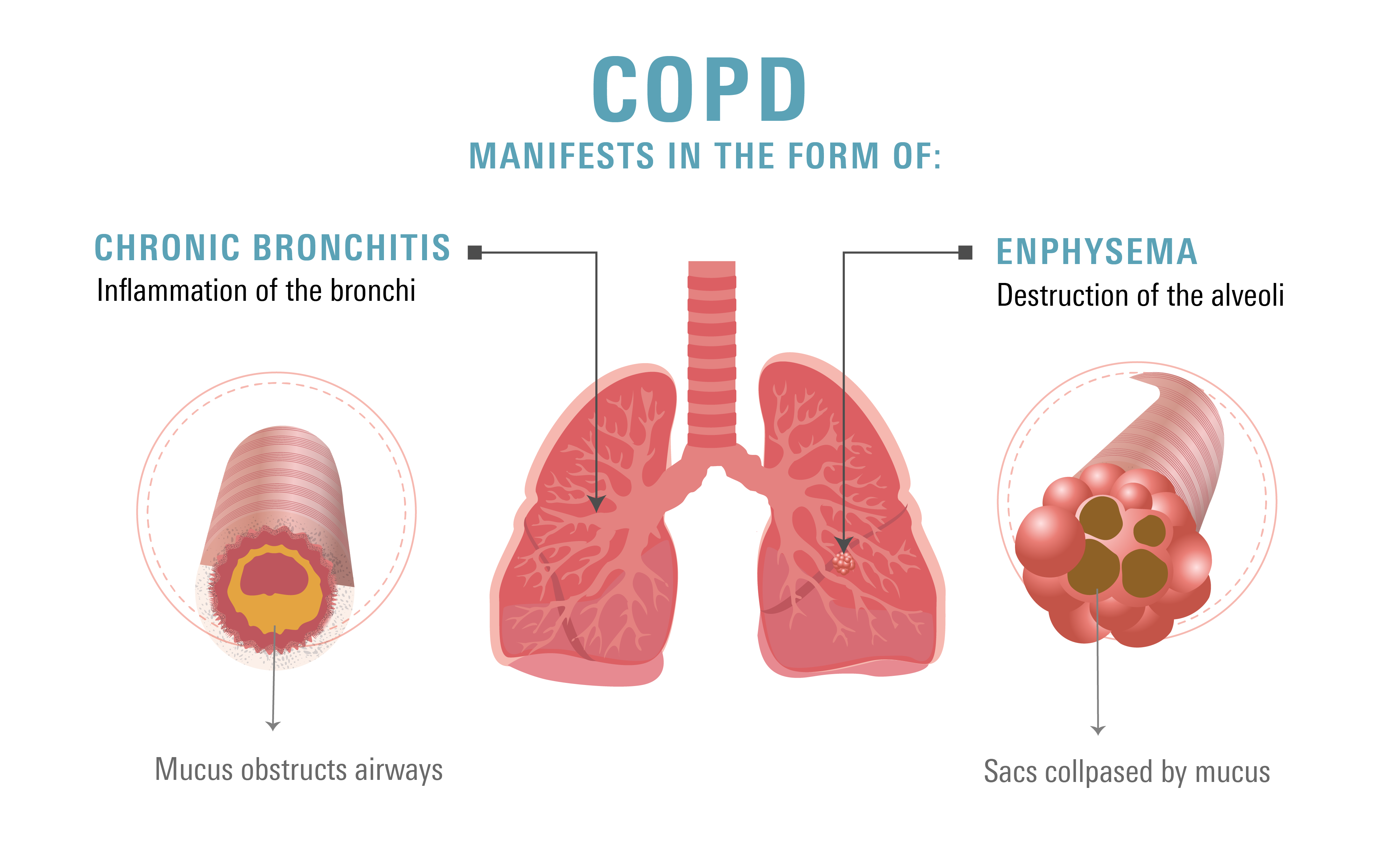
Two most common types of COPD
- Chronic bronchitis: defined as inflammation and narrowing of your bronchi tubes, resulting in mucus production and a chronic cough. May persist for at least 3 months for 2 years consecutively.
- Emphysema: is defined as the destruction of the small passages/air sacs in your lungs called alveoli. Your lungs may expand out and lose their springiness if your alveoli are damaged. You experience shortness of breath when air gets trapped in the lungs, making it difficult to exhale.
What Causes COPD?
The most frequent cause is chronic exposure to allergens that irritate your lungs. Smoking (smoking history of at least 10 years) is the main cause, but it can also be triggered by other air pollutants: noxious particles, smoke from fires, cigars, pipes, marijuana.
Chronic/long-term exposure to gases or particles leads to chronic inflammation in your lungs, and eventually emphysema and/or bronchitis.
What are the Symptoms of COPD?
You might not experience any symptoms in the beginning. But if the condition worsens, you can get the following symptoms:
- Dyspnea (shortness of breath) that’s chronic and progressive/worsens overtime
- Chronic cough
- Excessive saliva and mucus production
- Blue fingernail beds
- Wheezing
- Decreased energy
- Swollen ankles, feet, and/or legs
- Weight loss
- Chest tightness
People with COPD are also susceptible to exacerbations—symptoms worsen and last for at least a few days. If you have 2 or more exacerbations per year, you are considered to be a “frequent exacerbator.” Your risk of exacerbations increases as airflow limitations worsens.
It's critical to rule out other frequently occurring causes of cough and shortness of breath, such as asthma, chronic heart failure, and other lung diseases like tuberculosis. The most challenging disease to distinguish from COPD is asthma.
Learn more about asthma and medication options.
How is COPD Treated?
Effective treatments can control your symptoms, delay disease progression, lower your risk of complications and exacerbations, and improve your ability to lead an active life, even for more advanced stages of COPD.
Smoking cessation is the only management strategy proven to slow the progression of COPD. You can prevent COPD from progressing and losing your ability to breathe by quitting smoking.
Bronchodilator medications (inhalers)
Short-acting beta-2 agonist (SABA)—use as needed
- Albuterol (ProAir HFA, ProAir RespiClick, Proventil HFA, Ventolin HFA, ProAir Digihaler): MDI/DPI: 1–2 inhalations every 4–6 hours as needed
- Levalbuterol (Xopenex, Xopenex concentration, Xopenex HFA): MDI: 1-2 inhalations every 4–6 hours as needed
- Epinephrine (Primatene mist): MDI: 1–2 inhalations every 4 hours as needed. Available as an over-the-counter (OTC) medication
- Common side effects
- Nervousness
- Tremor
- Fast heart rate
- Palpitations
- Cough
- High blood sugar (hyperglycemia)
- High blood potassium levels
Short-acting muscarinic antagonist (SAMA)—use as needed
- Ipratropium Bromide (brand: Atrovent HFA): MDI: 2 inhalations four times a day
- Ipratropium Bromide + Albuterol (available as a brand: Combivent Respimat): MDI: 1 inhalation four times a day
- Common side effects
- Dry mouth
- Upper respiratory tract infections
- Cough
- Bitter taste
Long-acting beta-2 agonists—if regular use is required
- Salmeterol (Serevent Diskus): DPI: 1 inhalation twice a day
- Salmeterol + Fluticasone (Advair Diskus, Wixela Inhub): DPI: 1 inhalation twice a day
- Formoterol (Perforomist): Nebulizer solution: 20 mcg twice a day
- Formoterol + Budesonide (Symbicort)
- Formoterol + Aclidinium (Duaklir Pressair)
- Formoterol + Glycopyrrolate (Bevespi Aerosphere)
- Arformoterol (Brovana): Nebulizer solution: 15 mcg twice a day
- Indacaterol (Arcapta Neohaler): DPI: 1 capsule via Neohaler device daily.
The capsule is placed into the device. Do not swallow it. - Olodaterol (Striverdi Respimat): MDI: 1 inhalation daily
- Vilanterol + Fluticasone (Breo Ellipta)
- Vilanterol + Umeclidinium (Anoro Ellipta)
- Vilanterol + Umeclidinium/Fluticasone (Trelegy Ellipta)
- Common side effects
- Nervousness
- Tremor
- Increased heart rate
- Palpitations
- Hyperglycemia (high blood sugar)
- Cough
- Low potassium
Long-acting muscarinic antagonists (LABA)—if regular use is required
- Aclidinium (Tudorza Pressair): DPI: 1 inhalation twice a day
This medication has an indicator window that turns from green to red if the dose was inhaled properly. - Aclidinium + Formoterol (Duaklir Pressair): DPI: 1 inhalation twice a day
- Glycopyrrolate (Seebri Neohaler): DPI: 1 capsule via Neohaler device twice a day
This medication comes with a capsule that’s placed into the device. Do not swallow. - Revefenacin (Yupelri): Nebulizer: 175 mcg (1-unit dose vial) daily
- Umeclidinium (Incruse Ellipta): DPI: 1 inhalation daily
- Tiotropium (Spiriva Handihaler, Spiriva Respimat)
Spiriva Handihaler: DPI: 1 capsule via Handihaler device daily (requires 2 puffs). This medication is comes with a capsule that’s placed into the device. Do not swallow.
Spiriva Respimat: MDI: 2 inhalations daily - Common side effects
- Dry mouth
- Upper respiratory tract infections
- Cough
- Bitter taste
Inhaled Corticosteroids (ICS)
Can be added to LABA treatment or LAMA/LABA treatment for people with past exacerbations and high blood eosinophils (eos) counts (a marker of inflammation).
Although there’s a risk of pneumonia, adding an ICS has been shown to improve symptoms, lung function, quality of life, and reduce exacerbation frequency.
- Beclomethasone (QVAR RediHaler): MDI: 1-4 inhalations twice a day
- Budesonide (Pulmicort Flexhaler, Pulmicort Respules): DPI: 1-4 inhalations twice a day
- Ciclesonide (Alvesco): MDI: 1–2 inhalations twice a day
- Fluticasone (Flovent HFA, Flovent Diskus, Flovent Ellipta)
Flovent HFA: MDI: 2 inhalations twice a day
Flovent Diskus: DPI: 1–2 inhalations twice a day—Flovent Ellipta: DPI: 1-2 inhalations daily - Fluticasone + Salmeterol (Advair Diskus, Advair HFA, AirDuo RespiClick, Wixela Inhub)
- Mometasone (Asmanex HFA, Asmanex Twisthaler)
Asmanex HFA: MDI: 1–2 inhalations twice a day—Asmanex Twisthaler: DPI: 1–2 inhalations daily - Common side effects
- Difficulty speaking
- Cough
- Headache
- Hyperglycemia (high blood sugar)
- Hoarseness (raspy or strained voice)
- Oral candidiasis, also known as thrush.
Oral thrush is a fungus infection in the mouth.
To prevent oral thrush, rinse your mouth and throat with warm water and spit it out after each use, or use a spacer device if using an MDI.
All metered dose inhalers (MDI) are aerosol-based inhalers and should be shaken well before use.
All dry powder inhalers (DPI) deliver medications to your lungs in the form of dry powder.
Speak With Your Doctor
There is no cure for COPD. The best way to prevent COPD from progressing is to take good care of yourself. Talk to your healthcare provider today and send your prescription to Marley Drug. Save up to 95% compared to your local pharmacy by using Marley Drug.